- Home
- Author's Archive:
Vitamin D Deficiency Symptoms That Affect Energy, Immunity, and Mood
Vitamin D Deficiency Symptoms That Affect Energy, Immunity, and Mood
Vitamin D is a fat-soluble nutrient that helps the body absorb calcium and supports bone, muscle, immune, and nervous system function. The body can make vitamin D when skin is exposed to sunlight, and it can also come from foods and supplements. However, deficiency is common, especially in people with limited sun exposure, darker skin, certain digestive conditions, older age, or diets low in vitamin D.
Common vitamin D deficiency symptoms
Vitamin D deficiency does not always cause obvious symptoms at first. When symptoms do appear, they may include:
- Fatigue or low energy
- Muscle aches, cramps, or weakness
- Bone pain, especially in the back, hips, legs, or ribs
- Frequent infections or slower recovery from illness
- Low mood, irritability, or seasonal mood changes
- Poor sleep quality in some people
- Hair shedding, though this can have many causes
- Slow wound healing
These symptoms can overlap with many other conditions, including anemia, thyroid disease, depression, sleep disorders, chronic infections, and other vitamin deficiencies. A blood test is the most reliable way to confirm low vitamin D.
How low vitamin D may affect energy
Fatigue is one of the most commonly reported symptoms associated with vitamin D deficiency. Low vitamin D may contribute to tiredness indirectly by affecting muscle function, inflammation, sleep quality, or overall health. Some people describe the fatigue as feeling unusually heavy, persistent, or not fully relieved by rest.
Because fatigue has many possible causes, vitamin D should be considered as one part of a broader health evaluation rather than assumed to be the only explanation.
How deficiency can affect muscles and bones
Vitamin D helps regulate calcium and phosphorus, which are essential for strong bones. When vitamin D is too low, the body may have trouble maintaining normal bone mineralization. In adults, prolonged deficiency can contribute to osteomalacia, a condition that can cause bone pain and muscle weakness. In children, severe deficiency can lead to rickets.
Muscle symptoms may include weakness, cramps, tenderness, or difficulty with activities such as climbing stairs or getting up from a chair. Older adults with low vitamin D may also have a higher risk of falls, especially when muscle weakness is present.
Vitamin D and immune health
Vitamin D plays a role in immune system regulation. People with low vitamin D may notice they get sick more often, take longer to recover, or feel run down after infections. Research continues to study the relationship between vitamin D status and respiratory infections, but vitamin D is not a cure or guaranteed prevention for colds, flu, or other infections.
Maintaining adequate vitamin D is best viewed as part of a complete immune-supportive lifestyle that also includes sleep, nutrition, vaccination when appropriate, movement, and managing chronic conditions.
Vitamin D deficiency and mood changes
Low vitamin D has been associated with mood symptoms such as low mood, reduced motivation, irritability, and seasonal mood changes. This does not mean vitamin D deficiency is the sole cause of depression or anxiety, but it may be one factor worth evaluating, particularly when symptoms occur alongside fatigue, muscle aches, or limited sun exposure.
Anyone experiencing persistent sadness, loss of interest, thoughts of self-harm, or major changes in sleep, appetite, or functioning should seek professional mental health support promptly.
Who is at higher risk of vitamin D deficiency?
You may be more likely to have low vitamin D if you:
- Spend little time outdoors or cover most of your skin when outside
- Live in a northern climate or have limited winter sunlight
- Have darker skin, which reduces vitamin D production from sunlight
- Are an older adult
- Have obesity, which can affect vitamin D availability in the body
- Follow a diet low in vitamin D-rich foods
- Have conditions that affect fat absorption, such as celiac disease, Crohn’s disease, or certain liver or pancreatic disorders
- Have had bariatric surgery
- Take certain medications that affect vitamin D metabolism
- Are breastfed as an infant without recommended supplementation
How vitamin D deficiency is diagnosed
Healthcare providers usually check vitamin D status with a blood test called 25-hydroxyvitamin D. Your provider can interpret the result based on your health history, symptoms, risk factors, and local clinical guidelines.
It is not a good idea to take high-dose vitamin D without medical guidance. Too much vitamin D can cause toxicity, leading to high calcium levels, nausea, vomiting, weakness, confusion, kidney stones, and kidney damage.
Food sources of vitamin D
Vitamin D is found naturally in relatively few foods. Sources include:
- Fatty fish such as salmon, trout, tuna, and sardines
- Egg yolks
- Beef liver in small amounts
- Fortified milk or plant milks
- Fortified breakfast cereals
- Fortified orange juice in some regions
Sunlight can also help the body produce vitamin D, but safe sun exposure varies by skin type, location, season, age, and skin cancer risk. Sunscreen remains important for reducing skin damage.
When to talk to a healthcare provider
Consider asking about vitamin D testing if you have persistent fatigue, muscle weakness, bone pain, frequent infections, mood changes, or risk factors for deficiency. You should also seek medical advice before supplementing if you have kidney disease, high calcium levels, sarcoidosis, hyperparathyroidism, a history of kidney stones, or if you take medications that may interact with supplements.
Key takeaway
Vitamin D deficiency symptoms can affect energy, immunity, mood, muscles, and bones, but they are often nonspecific. If you suspect low vitamin D, the best next step is to discuss symptoms and testing with a healthcare professional. Correcting a deficiency safely can support overall health, but the right dose depends on your lab results, health status, and individual risk factors.
References
NIH Office of Dietary Supplements: Vitamin D Fact Sheet for Consumers
Anti Inflammatory Herbs and How They May Support Daily Wellness
Anti Inflammatory Herbs and How They May Support Daily Wellness
Inflammation is part of the body’s natural defense system. Short-term inflammation helps the body respond to injury or infection, but ongoing inflammation may be linked with many chronic health concerns. Daily habits such as balanced eating, regular movement, quality sleep, stress management, and avoiding tobacco all play important roles in supporting a healthy inflammatory response.
Anti inflammatory herbs may complement these habits. Many herbs contain plant compounds such as polyphenols, flavonoids, terpenes, and sulfur-containing compounds that have been studied for their potential effects on oxidative stress and inflammation-related pathways.
What Are Anti Inflammatory Herbs?
Anti inflammatory herbs are culinary or medicinal plants that contain naturally occurring compounds studied for their potential to influence inflammation. They are commonly used as spices, teas, extracts, or supplements.
It is important to keep expectations realistic. Eating herbs in food can support a nutrient-rich diet, but herbs are not a stand-alone treatment for inflammatory diseases. The strength, safety, and evidence vary widely depending on the herb, dose, preparation, and individual health status.
Common Anti Inflammatory Herbs
Turmeric
Turmeric contains curcumin, a yellow plant compound widely studied for its potential anti inflammatory and antioxidant properties. Turmeric is commonly used in curries, soups, rice dishes, smoothies, and warm drinks.
Curcumin is not absorbed very well on its own. It is often paired with black pepper, which contains piperine, or with dietary fat to improve absorption. However, concentrated turmeric or curcumin supplements may interact with blood thinners and may not be appropriate for everyone.
Ginger
Ginger is a warming root often used in teas, stir-fries, soups, and baked dishes. It contains compounds such as gingerols and shogaols that have been studied for effects related to inflammation, digestion, and nausea.
For daily wellness, ginger can be grated into meals, steeped as tea, or added to dressings and marinades. People taking blood-thinning medications or preparing for surgery should ask a healthcare professional before using high-dose ginger supplements.
Garlic
Garlic contains sulfur compounds, including allicin-related compounds, that have been studied for cardiovascular and immune-supporting effects. It is easy to add to vegetables, beans, soups, sauces, and whole-grain dishes.
Garlic supplements can be much stronger than culinary garlic and may increase bleeding risk in some people, especially when combined with anticoagulant or antiplatelet medications.
Cinnamon
Cinnamon is rich in polyphenols and is often used in oatmeal, yogurt, fruit, tea, and baked foods. It has been studied for possible effects on blood sugar regulation and inflammation-related markers.
There are different types of cinnamon. Cassia cinnamon contains coumarin, which may be harmful to the liver in large amounts. Using cinnamon as a food seasoning is generally different from taking concentrated supplements.
Rosemary
Rosemary is an aromatic herb containing compounds such as rosmarinic acid and carnosic acid. It pairs well with roasted vegetables, potatoes, beans, fish, poultry, and olive oil-based dishes.
Rosemary used in normal culinary amounts is common in many diets. Concentrated rosemary extracts or essential oils should be used cautiously and only with appropriate guidance.
Green Tea
Although often considered a beverage rather than an herb, green tea contains catechins such as EGCG, which have been studied for antioxidant and anti inflammatory activity. Unsweetened green tea can be a simple daily beverage option.
Green tea does contain caffeine unless labeled decaffeinated. Green tea extracts are more concentrated and have been associated with liver safety concerns in some cases, so supplement use should be discussed with a clinician.
How to Use Anti Inflammatory Herbs in Daily Life
A practical approach is to use herbs consistently in meals rather than relying on large supplement doses. Small daily additions can make healthy foods more flavorful and easier to maintain.
Simple ideas include:
- Add turmeric and black pepper to soups, lentils, scrambled eggs, or roasted cauliflower.
- Steep fresh ginger in hot water with lemon.
- Use garlic in bean dishes, vegetable sautés, and tomato sauces.
- Sprinkle cinnamon on oatmeal, apples, or plain yogurt.
- Add rosemary to roasted vegetables or olive oil marinades.
- Replace sugary drinks with unsweetened green tea when appropriate.
Herbs Work Best With an Anti Inflammatory Lifestyle
Herbs may be helpful, but they are only one part of daily wellness. A broader anti inflammatory lifestyle often includes:
- Eating plenty of vegetables, fruits, legumes, whole grains, nuts, seeds, and healthy fats.
- Choosing omega-3-rich foods such as fatty fish, flaxseed, chia seeds, or walnuts.
- Limiting highly processed foods, excess added sugar, and heavy alcohol intake.
- Moving regularly in a way that fits your ability and health status.
- Prioritizing sleep and stress management.
- Managing chronic conditions with professional medical care.
Safety Considerations
Natural does not always mean risk-free. Herbs can affect the body in meaningful ways, especially in concentrated extracts or supplement forms.
Speak with a healthcare professional before using anti inflammatory herbs therapeutically if you:
- Take prescription medications, especially blood thinners, diabetes medications, blood pressure medications, or immune-suppressing drugs.
- Are pregnant, trying to become pregnant, or breastfeeding.
- Have liver disease, kidney disease, gallbladder disease, bleeding disorders, or an upcoming surgery.
- Have allergies to related plants or spices.
- Are considering high-dose capsules, tinctures, extracts, or essential oils.
Bottom Line
Anti inflammatory herbs such as turmeric, ginger, garlic, cinnamon, rosemary, and green tea may support daily wellness when used as part of a balanced diet and healthy lifestyle. The safest approach for most people is to enjoy them in normal culinary amounts, choose high-quality foods, and consult a healthcare professional before using concentrated supplements.
References
Appendix
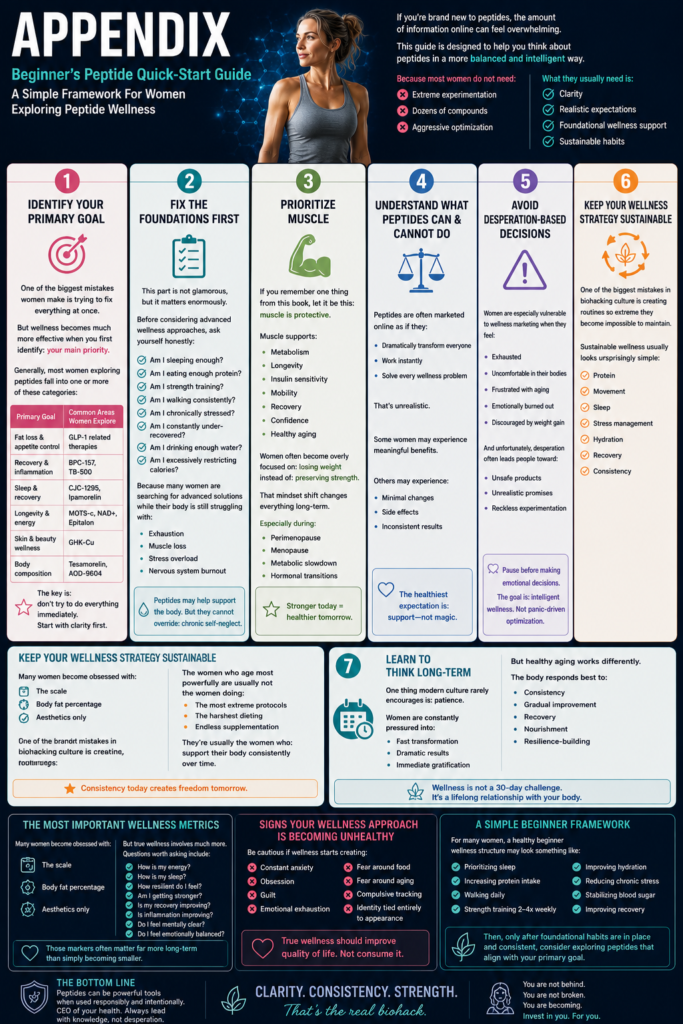
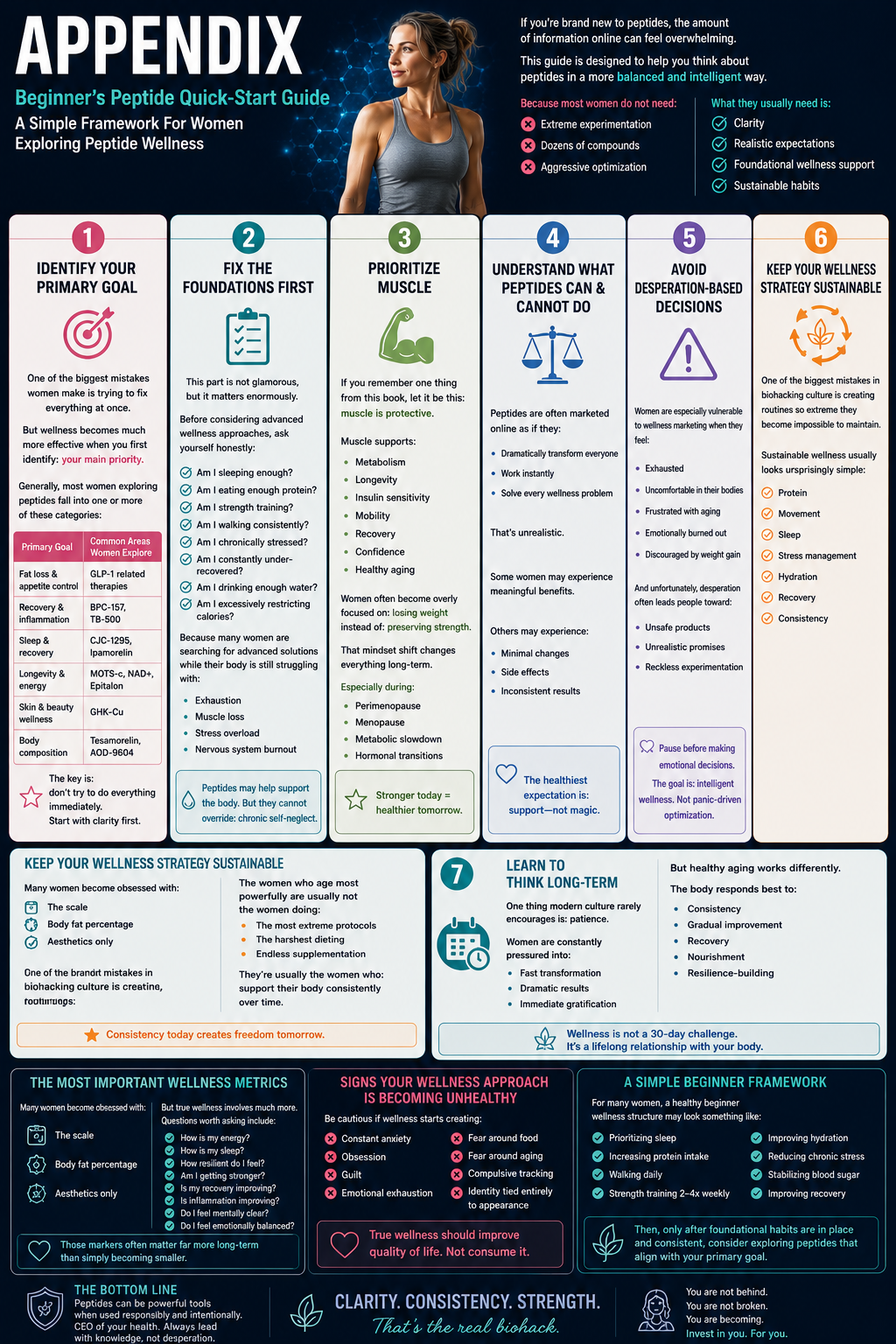
Beginner’s Peptide Quick-Start Guide
A Simple Framework For Women Exploring Peptide Wellness
If you’re brand new to peptides, the amount of information online can feel overwhelming very quickly.
Between:
- social media influencers
- biohacking podcasts
- wellness clinics
- Reddit forums
- aggressive marketing
- before-and-after photos
…it can become difficult to separate:
education from hype.
So before diving into advanced protocols or complicated stacks, I want to simplify the conversation as much as possible.
Because most women do not need:
- extreme experimentation
- dozens of compounds
- aggressive optimization
What they usually need is:
- clarity
- realistic expectations
- foundational wellness support
- sustainable habits
This guide is designed to help you think about peptides in a more balanced and intelligent way.
Step 1
Identify Your Primary Goal
One of the biggest mistakes women make is trying to fix:
everything at once.
But wellness becomes much more effective when you first identify:
your main priority.
Generally, most women exploring peptides fall into one or more of these categories:
| Primary Goal | Common Areas Women Explore |
| Fat loss & appetite control | GLP-1 related therapies |
| Recovery & inflammation | BPC-157, TB-500 |
| Sleep & recovery | CJC-1295, Ipamorelin |
| Longevity & energy | MOTS-c, NAD+, Epitalon |
| Skin & beauty wellness | GHK-Cu |
| Body composition | Tesamorelin, AOD-9604 |
The key is:
don’t try to do everything immediately.
Start with clarity first.
Step 2
Fix The Foundations First
This part is not glamorous, but it matters enormously.
Before considering advanced wellness approaches, ask yourself honestly:
- Am I sleeping enough?
- Am I eating enough protein?
- Am I strength training?
- Am I walking consistently?
- Am I chronically stressed?
- Am I constantly under-recovered?
- Am I drinking enough water?
- Am I excessively restricting calories?
Because many women are searching for advanced solutions while their body is still struggling with:
- exhaustion
- muscle loss
- stress overload
- nervous system burnout
Peptides may help support the body.
But they cannot override:
chronic self-neglect.
Step 3
Prioritize Muscle
If you remember one thing from this book, let it be this:
muscle is protective.
Muscle supports:
- metabolism
- longevity
- insulin sensitivity
- mobility
- recovery
- confidence
- healthy aging
Women often become overly focused on:
losing weight
instead of:
preserving strength.
That mindset shift changes everything long-term.
Especially during:
- perimenopause
- menopause
- metabolic slowdown
- hormonal transitions
Step 4
Understand What Peptides Can & Cannot Do
Peptides are often marketed online as if they:
- dramatically transform everyone
- work instantly
- solve every wellness problem
That’s unrealistic.
Some women may experience meaningful benefits.
Others may experience:
- minimal changes
- side effects
- inconsistent results
The healthiest expectation is:
support—not magic.
Step 5
Avoid Desperation-Based Decisions
Women are especially vulnerable to wellness marketing when they feel:
- exhausted
- uncomfortable in their bodies
- frustrated with aging
- emotionally burned out
- discouraged by weight gain
And unfortunately, desperation often leads people toward:
- unsafe products
- unrealistic promises
- reckless experimentation
Pause before making emotional decisions.
The goal is:
intelligent wellness.
Not panic-driven optimization.
Step 6
Keep Your Wellness Strategy Sustainable
One of the biggest mistakes in biohacking culture is creating routines so extreme they become impossible to maintain.
Sustainable wellness usually looks surprisingly simple:
- protein
- movement
- sleep
- stress management
- hydration
- recovery
- consistency
The women who age most powerfully are usually not the women doing:
- the most extreme protocols
- the harshest dieting
- endless supplementation
They’re usually the women who:
support their body consistently over time.
Step 7
Learn To Think Long-Term
One thing modern culture rarely encourages is:
patience.
Women are constantly pressured into:
- fast transformation
- dramatic results
- immediate gratification
But healthy aging works differently.
The body responds best to:
- consistency
- gradual improvement
- recovery
- nourishment
- resilience-building
Wellness is not a 30-day challenge.
It’s a lifelong relationship with your body.
The Most Important Wellness Metrics
Many women become obsessed with:
- the scale
- body fat percentage
- aesthetics only
But true wellness involves much more.
Questions worth asking include:
- How is my energy?
- How is my sleep?
- How resilient do I feel?
- Am I getting stronger?
- Is my recovery improving?
- Is inflammation improving?
- Do I feel mentally clear?
- Do I feel emotionally balanced?
Those markers often matter far more long-term than:
simply becoming smaller.
Signs Your Wellness Approach Is Becoming Unhealthy
Be cautious if wellness starts creating:
- constant anxiety
- obsession
- guilt
- emotional exhaustion
- fear around food
- fear around aging
- compulsive tracking
- identity tied entirely to appearance
True wellness should improve:
quality of life.
Not consume it.
A Simple Beginner Framework
For many women, a healthy beginner wellness structure may look something like:
- prioritizing sleep
- increasing protein intake
- walking daily
- strength training 2–4x weekly
- improving hydration
- reducing chronic stress
- stabilizing blood sugar
- improving recovery
Then, only after foundations improve:
- thoughtfully exploring advanced wellness options if appropriate.
That’s a far healthier long-term strategy than:
chasing shortcuts immediately.
The Truth About Healthy Aging
The women who tend to age best are rarely:
- the women punishing themselves hardest
or - the women obsessing over perfection
They are usually the women who:
- nourish themselves well
- maintain muscle
- stay physically active
- protect sleep
- preserve emotional balance
- remain curious and engaged with life
Healthy aging is not simply physical.
It’s deeply emotional too.
Ava’s Perspective
If I’ve learned anything through wellness, it’s this:
the body responds remarkably well to support.
Not punishment.
Not panic.
Not perfectionism.
The more I focused on:
- recovery
- nourishment
- strength
- sleep
- consistency
the better my body responded over time.
And honestly, I think many women are far more exhausted from fighting themselves than they realize.
Wellness should feel:
- empowering
- grounding
- sustainable
- life-giving
Not exhausting.
That’s the mindset I hope women carry with them long after finishing this book.
Quick-Start Summary
Focus on:
- Protein
- Sleep
- Muscle
- Recovery
- Walking
- Strength training
- Stress management
- Consistency
- Realistic expectations
Avoid:
- Panic-driven wellness
- Extreme restriction
- Overtraining
- Obsessive biohacking
- Unsafe sourcing
- Miracle-solution thinking
- Fear-based anti-aging culture
Educational Disclaimer
This book is intended for educational and informational purposes only.
It is not medical advice and should not replace consultation with qualified healthcare professionals.
Many peptides discussed in wellness and biohacking communities remain:
- investigational
- experimental
- incompletely studied for long-term human use
Women should discuss any peptide-related therapy, medication, supplement, or wellness intervention with appropriately licensed healthcare providers—especially if they have:
- medical conditions
- hormone-sensitive conditions
- metabolic disorders
- pregnancy or breastfeeding considerations
- complex health histories
Individual responses, risks, and outcomes vary significantly.
Always prioritize:
- safety
- evidence-informed decision making
- realistic expectations
- professional oversight
- high-quality sourcing
Your health deserves thoughtful, informed care.
Appendix B
Peptide Glossary
Simple Definitions For Common Terms Used In Wellness & Longevity Conversations
One of the most confusing parts of entering the peptide and longevity world is the language.
Women are suddenly exposed to terms like:
- GLP-1
- growth hormone secretagogues
- mitochondrial function
- visceral fat
- insulin sensitivity
- inflammation markers
- bioavailability
- peptide stacks
…and it can quickly feel overwhelming.
So this glossary is designed to simplify the most common concepts discussed throughout this book in plain, easy-to-understand language.
A
Amino Acids
Small molecules that act as the building blocks of protein. Peptides are made from chains of amino acids.
Appetite Regulation
The body’s system for controlling:
- hunger
- fullness
- cravings
- food intake
Several peptides discussed in wellness communities are associated with appetite-related signaling pathways.
AOD-9604
AOD-9604 — A peptide commonly discussed in fat-loss and metabolic wellness conversations.
B
BPC-157
BPC-157 — A peptide frequently discussed in wellness communities for recovery, inflammation, and tissue-support conversations.
Biohacking
A broad term used to describe intentional efforts to optimize:
- health
- performance
- recovery
- longevity
through lifestyle strategies, technology, supplements, or wellness interventions.
Biological Aging
The internal aging process occurring within cells and tissues, which may differ from chronological age.
C
Cellular Health
A broad wellness term referring to how efficiently and resiliently cells function throughout the body.
CJC-1295
CJC-1295 — A peptide commonly discussed in recovery, sleep, and longevity wellness conversations.
Collagen
A structural protein important for:
- skin elasticity
- connective tissue
- joints
- healthy aging appearance
Collagen production naturally declines with age.
Compounding Pharmacy
A specialized pharmacy that prepares customized medications under regulated guidelines.
Cortisol
Often called the “stress hormone.” Chronic elevation may contribute to:
- abdominal fat gain
- inflammation
- sleep disruption
- fatigue
D
Dosage Range
A general amount commonly discussed in research or wellness conversations. This book intentionally avoids specific dosing instructions.
E
Epitalon
Epitalon — A peptide commonly discussed in longevity and healthy-aging conversations.
Estrogen
A major female hormone involved in:
- metabolism
- mood
- skin health
- bone health
- body composition
Estrogen levels fluctuate significantly during perimenopause and menopause.
F
Fat Loss
Reduction in stored body fat. Healthy body composition involves preserving muscle while reducing excess fat.
Functional Wellness
A wellness approach focused on improving:
- energy
- mobility
- metabolism
- resilience
- quality of life
not simply appearance alone.
G
GHK-Cu
GHK-Cu — A copper peptide commonly discussed for skin, collagen, and regenerative wellness support.
GLP-1
Short for glucagon-like peptide-1.
A naturally occurring hormone involved in:
- appetite regulation
- blood sugar regulation
- fullness signaling
GLP-1-related medications became popular in weight-management conversations.
Growth Hormone
A naturally occurring hormone associated with:
- recovery
- muscle preservation
- metabolism
- tissue repair
Growth hormone naturally declines with age.
H
Hormonal Transition
Changes in hormone levels commonly occurring during:
- perimenopause
- menopause
- aging
These shifts may affect:
- energy
- body composition
- mood
- sleep
- metabolism
I
Inflammation
The body’s natural immune response.
Chronic inflammation may contribute to:
- fatigue
- pain
- metabolic dysfunction
- accelerated aging
Insulin Resistance
A condition where the body becomes less responsive to insulin, often contributing to:
- abdominal fat gain
- fatigue
- blood sugar instability
- metabolic dysfunction
Ipamorelin
Ipamorelin — A peptide commonly discussed in recovery and healthy-aging conversations.
L
Longevity
The study and pursuit of healthy aging, resilience, and maintaining quality of life over time.
M
Menopause
The natural biological transition marking the end of menstrual cycles.
Often associated with changes involving:
- metabolism
- sleep
- body composition
- energy
- inflammation
Metabolism
The body’s system for producing and using energy.
Metabolic health affects:
- body composition
- energy
- recovery
- blood sugar regulation
Mitochondria
Structures inside cells responsible for producing energy.
Often referred to as:
the “powerhouses” of the cell.
MOTS-c
MOTS-c — A peptide discussed in metabolic and longevity wellness conversations.
N
NAD+
Nicotinamide adenine dinucleotide — A coenzyme involved in cellular energy production and mitochondrial function.
Nervous System Regulation
Practices that help reduce chronic stress and support recovery.
Examples may include:
- sleep
- walking
- breathwork
- recovery practices
- stress management
P
Peptide
A short chain of amino acids that may influence biological signaling within the body.
Peptide Stack
Combining multiple peptides together for complementary wellness goals.
Perimenopause
The transitional years leading up to menopause, often involving hormonal fluctuations and symptoms such as:
- weight gain
- sleep changes
- mood shifts
- fatigue
Protein
An essential nutrient important for:
- muscle preservation
- metabolism
- recovery
- healthy aging
R
Recovery
The body’s repair and restoration process after:
- exercise
- stress
- illness
- inflammation
Resilience
The body’s ability to adapt to:
- stress
- aging
- recovery demands
- physical challenges
S
Semaglutide
Semaglutide — A medication commonly discussed for appetite regulation and weight management.
Sleep Quality
How restorative and uninterrupted sleep is.
Poor sleep may affect:
- metabolism
- inflammation
- hormones
- cravings
- recovery
Strength Training
Exercise focused on building or maintaining muscle.
One of the most important wellness habits for healthy aging.
T
Telomeres
Protective structures at the ends of chromosomes associated with cellular aging discussions.
Tesamorelin
Tesamorelin — A peptide commonly discussed in visceral fat and body composition conversations.
TB-500
TB-500 — A peptide discussed in mobility and recovery wellness conversations.
Tirzepatide
Tirzepatide — A medication discussed for metabolic wellness and appetite regulation.
V
Visceral Fat
Fat stored around internal organs within the abdominal cavity.
Excess visceral fat is associated with:
- metabolic dysfunction
- inflammation
- insulin resistance
W
Wellness Optimization
Intentional efforts to improve:
- energy
- recovery
- metabolism
- resilience
- healthy aging
through sustainable lifestyle and wellness strategies.
Final Glossary Note
You do not need to become a scientist to improve your health.
One of the biggest mistakes women make is believing they must:
- master every technical concept
- optimize every variable
- become obsessed with wellness
But true health rarely comes from:
perfection.
It usually comes from:
- consistency
- self-awareness
- recovery
- movement
- nourishment
- resilience
- sustainable habits practiced over time
And honestly, I think that mindset will carry women further than any advanced wellness trend ever could.
About The Author
Ava Laurent
Ava Laurent is a wellness writer and longevity enthusiast focused on helping women navigate:
- midlife health
- metabolism
- recovery
- healthy aging
- body composition
- energy optimization
- sustainable wellness
After years of struggling with:
- chronic stress
- burnout
- hormonal changes
- inflammation
- stubborn weight fluctuations
- exhaustion from restrictive wellness culture
…Ava became deeply interested in the science of:
- metabolic health
- recovery
- peptide wellness
- longevity
- resilience-focused aging
What began as personal curiosity eventually evolved into a passion for helping women better understand:
- their bodies
- healthy aging
- realistic wellness strategies
- the importance of muscle, sleep, recovery, and metabolic health
Rather than promoting:
- perfection
- punishment
- fear-based anti-aging
Ava believes wellness should focus on:
- vitality
- confidence
- resilience
- sustainable habits
- quality of life
Her philosophy combines:
- practical wellness
- evidence-informed education
- modern longevity conversations
- balanced biohacking
- realistic expectations
with a strong emphasis on:
supporting the body rather than fighting it.
A Personal Note From Ava
If you’ve read this book all the way through, I first want to say:
thank you.
Women today are overwhelmed with:
- conflicting wellness advice
- fear-based marketing
- impossible beauty standards
- endless pressure to optimize everything
And honestly, I think many women are exhausted from constantly feeling like they need fixing.
My hope with this book was never to convince women they need:
- more supplements
- more injections
- more obsession
- more perfection
My goal was to create a conversation around:
- informed wellness
- healthy aging
- resilience
- metabolic health
- realistic self-care
Because ultimately, I believe the healthiest women are usually the women who:
- nourish themselves well
- move consistently
- protect their sleep
- maintain muscle
- manage stress intelligently
- recover properly
- approach themselves with self-respect instead of criticism
Peptides may become part of that journey for some women.
But they should never replace:
- foundational health habits
- realistic expectations
- emotional wellbeing
- self-worth
You deserve wellness that helps you:
- feel energized
- feel confident
- feel capable
- feel alive
Not wellness rooted in fear.
Thank you for spending this time with me.
And wherever you are in your journey right now, I hope you move forward with:
- curiosity
- confidence
- balance
- resilience
- compassion for yourself and your body
Because healthy aging is not about becoming less.
It’s about continuing to become more fully yourself with time.
— Ava Laurent
Additional Educational Disclaimer
This book is intended strictly for educational and informational purposes only.
Nothing in this book should be interpreted as:
- medical advice
- diagnosis
- treatment recommendations
- individualized healthcare guidance
Many compounds discussed throughout this book remain:
- investigational
- experimental
- incompletely studied for long-term human use
Readers should consult qualified healthcare professionals before making decisions related to:
- medications
- peptides
- supplements
- hormone therapies
- metabolic health interventions
- wellness protocols
Especially if they have:
- medical conditions
- hormone-sensitive conditions
- cardiovascular disease
- metabolic disorders
- autoimmune conditions
- pregnancy or breastfeeding considerations
- complex medical histories
Neither the author nor publisher assumes responsibility for decisions made based on the material presented in this book.
Always prioritize:
- evidence-informed decision making
- realistic expectations
- professional oversight
- high-quality sourcing
- long-term health and safety
Your health deserves thoughtful, informed care.
Suggested Resources & Next Steps
For women interested in continuing their wellness journey, consider learning more about:
- strength training for women over 35
- metabolic health
- sleep optimization
- protein intake and muscle preservation
- stress management
- menopause education
- recovery-focused wellness
- evidence-based longevity research
Remember:
sustainable wellness almost always beats extreme wellness long-term.
And the goal is not:
perfection.
The goal is:
vitality, resilience, confidence, and quality of life for years to come.
Chapter 18: The Truth About Wellness, Aging & Your Body

A Final Conversation
If you’ve made it this far, you’ve probably realized something important:
this book was never really just about peptides.
Yes, we discussed:
- metabolism
- fat loss
- recovery
- longevity
- body composition
- inflammation
- healthy aging
But underneath all of that was a much bigger conversation:
how women experience their bodies as they age.
And honestly, I think that conversation matters far more than any individual peptide ever could.
Women Have Been Taught To Fight Their Bodies
For decades, women were taught that wellness meant:
- eating less
- exercising harder
- ignoring fatigue
- tolerating burnout
- shrinking themselves constantly
And if the body resisted?
Women were often told it was because they lacked:
- discipline
- willpower
- motivation
But the truth is:
the female body is biologically dynamic.
Hormones change.
Recovery changes.
Metabolism changes.
Stress tolerance changes.
Sleep changes.
And midlife often becomes the moment women finally realize:
they cannot bully their bodies into thriving.
That realization can feel frustrating at first.
But ultimately, I think it becomes liberating.
Because once women understand their bodies more deeply, they often stop approaching wellness through:
- punishment
- shame
- exhaustion
- self-criticism
And start approaching it through:
- support
- nourishment
- resilience
- intelligence
- sustainability
That shift changes everything.
The Wellness Industry Often Profits From Fear
One thing I want to say honestly is this:
modern wellness culture can become extremely manipulative.
Women are constantly told:
- they’re aging too fast
- they’re too tired
- they’re gaining too much weight
- they don’t look young enough
- they need fixing
And unfortunately, fear sells.
Especially fear around:
- aging
- body image
- attractiveness
- relevance
- femininity
But aging is not failure.
Aging is:
- human
- biological
- natural
The healthier goal is not:
trying to become ageless.
The healthier goal is:
becoming resilient, strong, energized, and healthy while aging.
That’s a profoundly different mindset.
Peptides Are Tools—Not Magic
One of the most important things I hope women understand is this:
peptides are tools.
Not miracles.
Some women may find certain peptide therapies genuinely helpful for:
- appetite regulation
- recovery
- inflammation support
- body composition
- sleep
- metabolic health
Others may not respond dramatically at all.
And no peptide can fully compensate for:
- chronic stress
- poor sleep
- muscle loss
- burnout
- sedentary living
- severe nutritional neglect
The body still needs:
- movement
- recovery
- nourishment
- protein
- sleep
- emotional wellbeing
- nervous system support
The basics still matter.
Probably more than ever.
Muscle Is One Of The Most Important Things Women Can Protect
If there’s one physical theme repeated throughout this book, it’s this:
muscle matters enormously.
Muscle supports:
- metabolism
- insulin sensitivity
- mobility
- strength
- recovery
- longevity
- independence later in life
And unfortunately, many women unknowingly sacrifice muscle through:
- under-eating
- excessive cardio
- chronic dieting
- fear of strength training
But healthy aging requires:
preserving strength.
Not simply becoming smaller.
That’s one of the healthiest mindset shifts women can make.
Recovery Is Not Laziness
Another thing modern women desperately need to hear:
recovery is productive.
The body cannot thrive in a constant state of:
- stress
- exhaustion
- inflammation
- overstimulation
- sleep deprivation
Yet many women normalize all of those things.
Recovery matters because:
- hormones recover during sleep
- muscle repairs during recovery
- metabolism stabilizes with nervous system balance
- inflammation improves when stress decreases
Women often believe they need more discipline.
Sometimes what they actually need is:
- more rest
- more nourishment
- more support
- less self-punishment
That distinction matters deeply.
Aging Can Become A Powerful Transition
One thing I’ve personally realized is that aging can actually become:
an awakening.
Many women enter midlife exhausted from:
- chasing impossible standards
- comparing themselves constantly
- trying to earn worth through appearance
And eventually they begin asking better questions:
- How do I want to feel?
- How do I protect my energy?
- How do I preserve my health long-term?
- How do I maintain vitality and confidence?
That shift creates far healthier relationships with wellness.
Because eventually:
quality of life matters more than perfection.
The Women Who Thrive Long-Term Usually Prioritize The Same Things
Over and over, the healthiest and most vibrant women tend to focus on:
- movement
- strength
- sleep
- protein
- stress management
- recovery
- meaningful relationships
- emotional balance
- consistency
Not perfection.
Not punishment.
Not obsession.
Just sustainable care for themselves over time.
And honestly, I think that’s one of the most powerful forms of self-respect a woman can practice.
Confidence Changes With Age
One of the most beautiful things about healthy aging is that confidence often becomes less performative.
You stop trying to:
- impress everyone
- meet impossible standards
- constantly prove yourself
And instead begin focusing on:
- feeling strong
- feeling healthy
- feeling grounded
- feeling capable
- feeling alive
That type of confidence tends to feel much more peaceful—and much more sustainable.
You Are Allowed To Care About Yourself
I also want women to understand this:
caring about your health and appearance is not shallow.
There is nothing wrong with wanting to:
- feel attractive
- maintain vitality
- support your skin
- improve body composition
- feel confident in your body
The healthiest approach is simply:
balance.
Not obsession.
Not shame.
Not fear.
Just intentional self-care rooted in respect for yourself and your future.
Wellness Should Expand Your Life—Not Consume It
At its best, wellness should help women:
- move more freely
- feel more energized
- enjoy life more deeply
- participate more fully
- maintain independence longer
- feel confident physically and emotionally
It should not create:
- constant anxiety
- obsessive tracking
- endless comparison
- fear around aging
- emotional exhaustion
True wellness creates:
freedom.
Not captivity.
What I Hope You Take Away From This Book
If there’s one message I hope stays with you, it’s this:
your body is not the enemy.
Your body is adapting continuously to:
- stress
- hormones
- aging
- recovery
- lifestyle
- inflammation
- nourishment
- sleep
- emotional health
And the more intelligently and compassionately you support it, the better it tends to respond over time.
You do not need:
- perfection
- punishment
- panic
You need:
- consistency
- education
- resilience
- strength
- recovery
- self-respect
That’s the foundation of healthy aging.
Ava’s Final Perspective
If I could tell every woman one thing, it would be this:
aging does not reduce your value.
You are not becoming less powerful.
Less beautiful.
Less worthy.
In many ways, women become:
- wiser
- stronger
- more emotionally grounded
- more resilient
- more self-aware with age
And I think wellness should support that evolution—not make women fear it.
To me, the goal is not to become ageless.
The goal is to become:
- healthy
- energetic
- strong
- capable
- confident
- fully alive
At every stage of life.
And honestly, I think that’s far more beautiful than perfection ever was.
Final Key Takeaways
True wellness should create freedom, resilience, energy, and quality of life.
Peptides are tools—not magic solutions.
Healthy aging requires muscle preservation, recovery, sleep, and metabolic health.
Women should approach wellness through support rather than punishment.
Aging is biological—not personal failure.
Sustainable wellness comes from consistency, not perfection.
Confidence and vitality matter more than unrealistic beauty standards.
Chapter 17: How To Source Peptides Safely

Quality, Legitimacy & Avoiding Dangerous Mistakes
One of the biggest questions women eventually ask after learning about peptides is:
“How do people actually obtain these?”
And honestly, this is where things become complicated.
Because while peptides have exploded in popularity across:
- wellness clinics
- longevity spaces
- social media
- biohacking communities
…the peptide industry itself is still highly fragmented.
Which means:
quality varies enormously.
And unfortunately, many women enter this space without realizing:
- products may be underdosed
- mislabeled
- contaminated
- improperly stored
- completely fake
This is why sourcing deserves serious attention.
Because no peptide conversation matters if:
the product itself is poor quality or unsafe.
Why The Peptide Industry Is So Confusing
Part of the confusion comes from the fact that peptides exist across several different categories:
- prescription medications
- compounded wellness products
- research-use products
- cosmetic formulations
- wellness clinic protocols
Some peptides have:
- FDA-approved medical uses
while others remain: - experimental
- research-focused
- not approved for general medical treatment
This creates enormous confusion for consumers trying to navigate the space safely.
Especially because social media often presents peptides as:
casual wellness products
without discussing:
- legality
- sourcing quality
- sterility
- safety standards
- medical oversight
The Biggest Mistake Women Make
One of the most dangerous mistakes women make is assuming:
all peptide suppliers are equal.
They are not.
In fact, quality differences can be dramatic.
And because peptides are biologically active compounds, poor-quality sourcing may create serious risks involving:
- contamination
- inaccurate labeling
- improper formulation
- bacterial exposure
- dosing inconsistency
This is one reason cautious sourcing matters so much.
The Safest General Approach
The most conservative and safety-focused approach is generally working through:
- licensed healthcare providers
- established medical clinics
- reputable compounding pharmacies when appropriate
- qualified longevity or metabolic health professionals
Women exploring peptides should ideally seek:
- transparency
- medical oversight
- ingredient accountability
- sterility standards
- quality testing
Especially for injectable products.
What Is A Compounding Pharmacy?
Food and Drug Administration-regulated compounding pharmacies prepare customized medications under specific regulatory frameworks.
In wellness and longevity settings, some peptide-related therapies may be obtained through properly licensed compounding pharmacies working alongside healthcare providers.
Women often prefer this route because it may provide:
- better quality assurance
- sterility standards
- dosing consistency
- medical guidance
- prescription oversight
However, regulations and availability vary by:
- state
- country
- peptide category
- current regulatory environment
Which is why professional guidance matters.
Why “Cheap” Can Become Dangerous
One thing I strongly encourage women to avoid is making decisions based solely on:
price.
Cheap peptide products may carry significantly higher risks involving:
- contamination
- improper storage
- inaccurate concentration
- poor manufacturing standards
And unfortunately, online wellness culture often encourages:
- bargain hunting
- underground sourcing
- impulsive experimentation
without adequately discussing risk.
That’s a problem.
Because injectable products require:
- sterility
- proper handling
- manufacturing quality
- careful sourcing
Red Flags To Watch For
Women should be cautious of suppliers that:
- make unrealistic promises
- guarantee dramatic results
- lack transparency
- avoid discussing testing
- provide no quality documentation
- aggressively market “miracle” outcomes
- appear anonymous or unprofessional
Extreme marketing hype is often a warning sign.
Especially in wellness spaces.
Why Lab Testing Matters
Reputable peptide discussions often involve concepts such as:
- third-party testing
- purity verification
- sterility testing
- batch consistency
This matters because peptides are sensitive compounds.
Improper handling or manufacturing may affect:
- stability
- potency
- safety
Again:
quality matters enormously.
Especially with anything injected into the body.
The Social Media Problem
One thing that concerns me about modern wellness culture is how casually peptides are often discussed online.
Influencers may present peptide use as:
- effortless
- risk-free
- universally effective
while completely skipping conversations around:
- medical oversight
- contraindications
- sourcing risks
- side effects
- long-term unknowns
That creates unrealistic expectations and sometimes unsafe behavior.
Especially among women feeling vulnerable about:
- aging
- body image
- chronic fatigue
- weight struggles
Women deserve honest education—not exaggerated hype.
The Emotional Vulnerability Factor
One thing wellness marketers understand extremely well is this:
women who feel exhausted or frustrated are often emotionally vulnerable.
Women struggling with:
- weight gain
- menopause symptoms
- fatigue
- chronic pain
- body changes
may feel desperate for solutions.
And unfortunately, desperation sometimes leads people toward:
- unsafe products
- aggressive claims
- unrealistic expectations
This is one reason balanced education matters so much.
Women should never feel pressured into:
- reckless experimentation
- shame-based wellness
- fear-driven purchasing
Questions Women Should Ask Before Using Peptides
Before exploring peptide-related wellness, women should thoughtfully consider:
- What are my actual goals?
- Do I understand the risks and unknowns?
- Am I prioritizing foundational health habits?
- Is this approach medically appropriate for me?
- Am I seeking support or chasing unrealistic transformation?
- Is the source reputable and transparent?
- Do I have realistic expectations?
These questions create much healthier decision-making.
Why Foundational Health Still Comes First
One of the biggest misconceptions in wellness culture is believing advanced therapies can override poor lifestyle habits.
They cannot.
No peptide can fully compensate for:
- chronic sleep deprivation
- unmanaged stress
- severe muscle loss
- inactivity
- poor nutrition
- excessive alcohol
- burnout
Women often want advanced solutions when they actually need:
- recovery
- protein
- sleep
- movement
- nervous system support
- metabolic stabilization
That doesn’t make peptides useless.
It simply means:
fundamentals still matter most.
The Most Sustainable Wellness Mindset
The healthiest women I know tend to approach wellness with:
- curiosity
- patience
- realism
- self-respect
- consistency
Not desperation.
Not obsession.
Not panic around aging.
And honestly, I think that emotional approach matters just as much as any supplement, peptide, or wellness strategy ever will.
Because stress itself profoundly affects:
- hormones
- inflammation
- recovery
- metabolism
- aging
Wellness should reduce chaos—not increase it.
The Difference Between Empowerment & Hype
True wellness education should empower women to:
- ask better questions
- make informed decisions
- understand their bodies
- think critically
- approach aging intelligently
It should not:
- manipulate insecurity
- promise miracles
- create fear
- encourage reckless behavior
That distinction matters enormously.
Especially in today’s wellness industry.
Ava’s Perspective
If there’s one thing I hope women take away from this book, it’s this:
your body deserves respect—not punishment.
You do not need to:
- panic about aging
- obsess over perfection
- chase every new trend
- experiment recklessly
Healthy aging is not about becoming flawless.
It’s about becoming:
- resilient
- informed
- strong
- energized
- confident
- intentional
And the women who tend to age most powerfully are usually the women who approach wellness from:
self-respect instead of fear.
That mindset changes everything.
Key Takeaways
- Peptide quality and sourcing matter enormously.
- Not all peptide suppliers are safe or reputable.
- Women should prioritize transparency, testing, and professional oversight.
- Cheap or poorly sourced products may carry serious risks.
- Social media often oversimplifies peptide safety and effectiveness.
- Foundational health habits still matter more than advanced wellness tools.
Sustainable wellness should be rooted in education, realism, and self-respect.
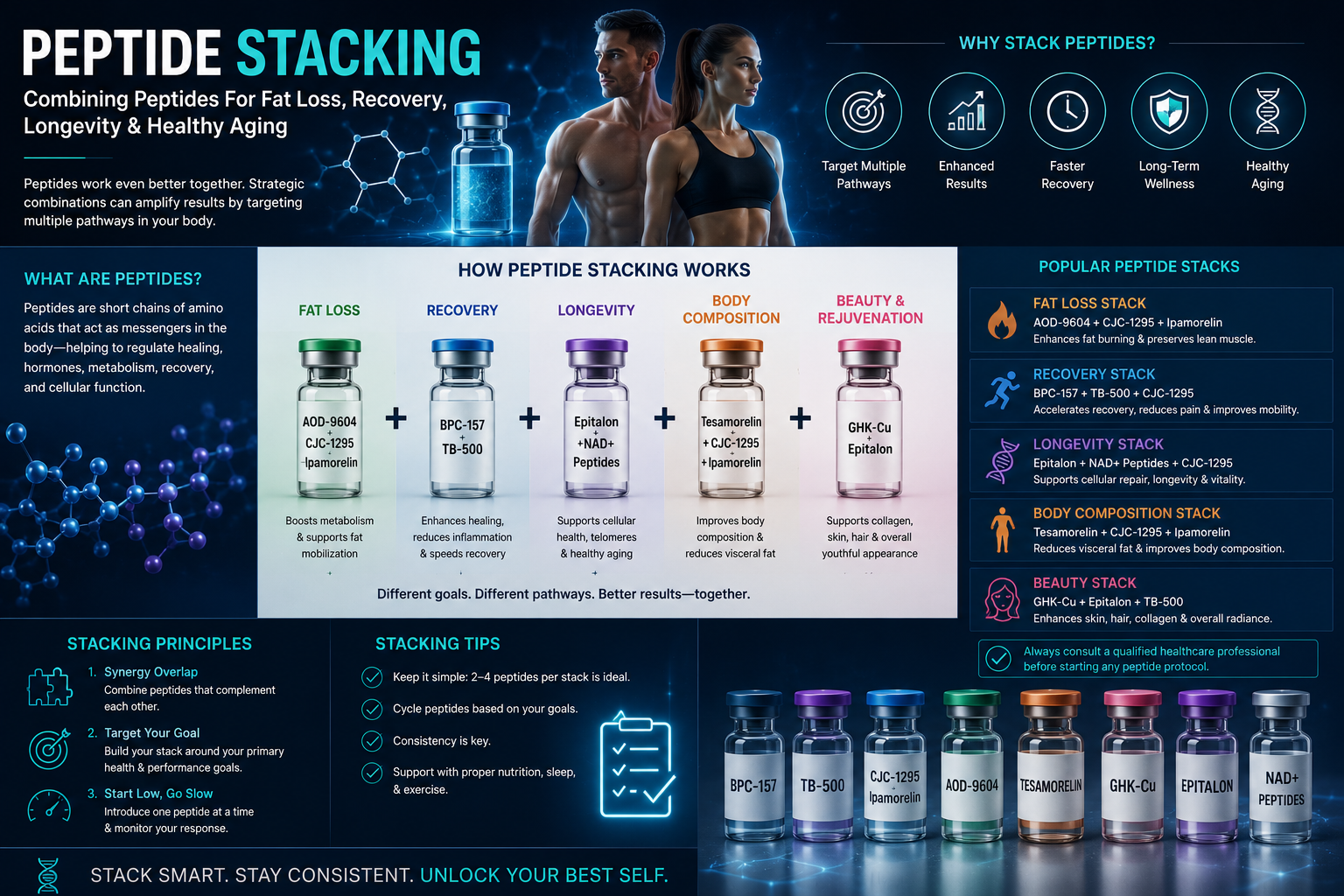
Chapter 16: Peptide Stacking
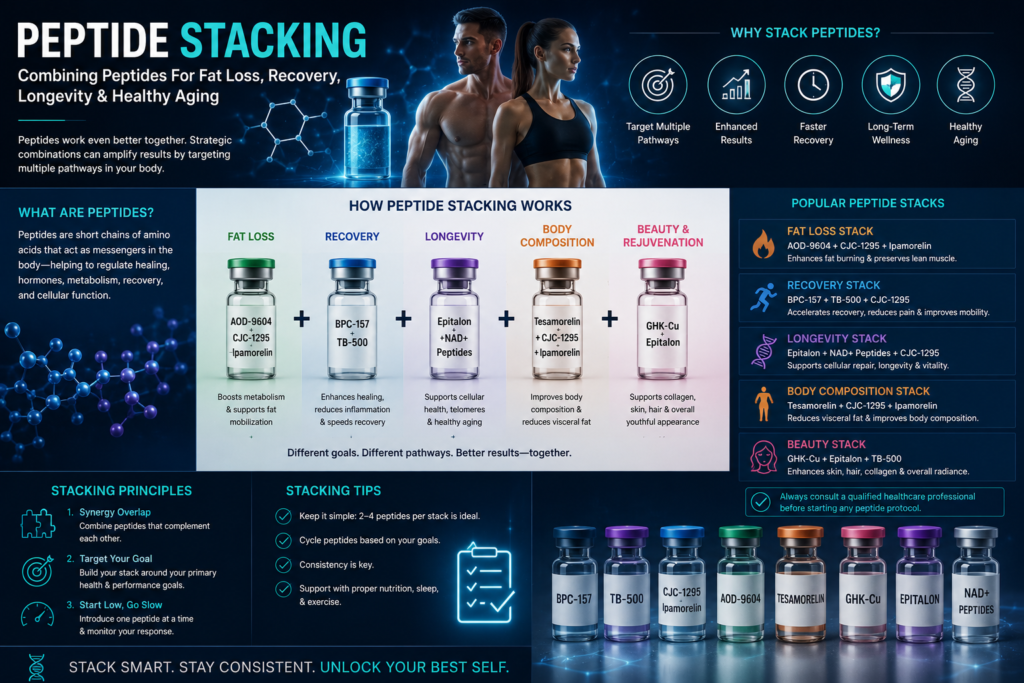

Combining Peptides For Fat Loss, Recovery, Longevity & Healthy Aging
Once women begin learning about peptides, one of the first questions that naturally comes up is:
“Can these peptides be combined together?”
In wellness and longevity communities, this is commonly referred to as:
peptide stacking.
A peptide stack simply means combining multiple peptides with different goals or mechanisms in mind.
For example:
- one peptide may focus on appetite regulation
- another may support recovery
- another may support sleep or body composition
The idea is to create a more comprehensive wellness strategy rather than relying on one compound alone.
And honestly, this makes sense.
Because real wellness is rarely about solving only one issue.
Women navigating midlife are often dealing with several overlapping challenges simultaneously:
- weight gain
- inflammation
- poor sleep
- reduced recovery
- low energy
- hormonal changes
- muscle loss
- stress
- metabolic slowdown
Which is why stacking conversations became so popular in:
- longevity clinics
- wellness communities
- biohacking culture
- metabolic optimization discussions
Important Reality Check Before Discussing Stacks
Before we talk about common peptide combinations, it’s important to say this clearly:
more is not always better.
One of the biggest mistakes in wellness culture is assuming that:
- adding more compounds
- taking more supplements
- aggressively optimizing everything
automatically creates better results.
It doesn’t.
In fact, excessive stacking can sometimes:
- increase side effects
- complicate recovery
- create unnecessary stress on the body
- make it harder to identify what’s actually helping
The healthiest wellness strategies tend to be:
thoughtful, intentional, and sustainable.
That mindset matters enormously.
The Most Common Reasons Women Explore Stacking
Women typically become interested in peptide stacks for four major reasons:
- Fat loss & metabolic support
- Recovery & inflammation reduction
- Sleep & healthy aging
- Body composition & longevity optimization
Let’s break down the most common wellness-oriented approaches.
Stack #1
Metabolic & Fat Loss Support
Commonly Discussed Combination:
- Semaglutide or Tirzepatide
paired with: - AOD-9604
Why Women Explore This Combination
This type of stack is often discussed by women focused on:
- appetite control
- metabolic support
- body composition
- reducing stubborn abdominal fat
The idea is that:
- appetite-regulating peptides may help reduce cravings and overeating
while: - AOD-9604 is discussed in relation to fat metabolism support
Again, results vary considerably between individuals.
Important Considerations
Women using metabolic-focused stacks should pay close attention to:
- protein intake
- muscle preservation
- hydration
- resistance training
- nutrient quality
Rapid weight loss without muscle preservation may create:
- weakness
- metabolic slowdown
- fatigue
- poor long-term outcomes
Healthy body composition is not simply:
losing weight quickly.
It’s maintaining:
- strength
- resilience
- metabolic health
Stack #2
Recovery & Inflammation Support
Commonly Discussed Combination:
- BPC-157
paired with: - TB-500
Why Women Explore This Combination
This is one of the most commonly discussed recovery-focused stacks in wellness communities.
Women often become interested in it for:
- chronic soreness
- recovery support
- mobility
- tendon-related concerns
- inflammation support
- exercise recovery
Especially among women who want to:
- stay active
- maintain mobility
- continue strength training
- improve recovery consistency
The Bigger Wellness Lesson
One thing I find incredibly important here is that:
recovery is becoming mainstream wellness.
For years, women were taught to constantly:
- push harder
- exercise more
- ignore fatigue
- normalize exhaustion
But sustainable wellness depends heavily on:
- recovery
- nervous system regulation
- inflammation management
- resilience
That shift is long overdue.
Stack #3
Sleep, Recovery & Healthy Aging
Commonly Discussed Combination:
- CJC-1295
paired with: - Ipamorelin
Why Women Explore This Combination
Women interested in:
- sleep quality
- recovery
- healthy aging
- muscle preservation
- vitality
often become interested in this pairing.
Many women navigating midlife feel:
- under-recovered
- physically depleted
- chronically fatigued
This stack is often discussed within:
- longevity-focused wellness
- anti-aging conversations
- recovery optimization
Why Sleep Matters So Much
Sleep is deeply connected to:
- metabolism
- recovery
- appetite regulation
- cognitive function
- inflammation
- hormone balance
Many women underestimate how dramatically poor sleep affects:
- body composition
- cravings
- emotional resilience
- energy
Which is why recovery-focused wellness matters so much during midlife.
Stack #4
Longevity & Cellular Health
Commonly Discussed Combination:
- MOTS-c
paired with: - NAD+-focused wellness approaches
and occasionally: - Epitalon
Why Women Explore This Combination
This category is typically discussed by women focused on:
- energy
- longevity
- cellular health
- vitality
- healthy aging
- resilience
These conversations are especially popular in:
- biohacking communities
- longevity clinics
- advanced wellness spaces
The emphasis here is less about:
dramatic transformation
and more about:
maintaining function and vitality long-term.
Stack #5
Beauty, Recovery & Regeneration
Commonly Discussed Combination:
- GHK-Cu
paired with: - recovery-focused wellness
- collagen-supportive lifestyles
- metabolic optimization
Why Women Explore This Combination
Women interested in:
- skin quality
- healthy aging
- collagen support
- hair vitality
- regenerative wellness
often become interested in beauty-oriented peptide conversations.
And honestly, I think it’s important to normalize the idea that:
women can care about appearance without it being shallow.
Wanting to:
- look healthy
- feel confident
- age gracefully
is completely reasonable.
The Biggest Mistake In Biohacking Culture
One thing I’ve noticed repeatedly is that many people become obsessed with:
optimization overload.
They:
- chase too many compounds
- constantly switch protocols
- overcomplicate wellness
- ignore foundational health habits
But sustainable wellness almost always comes back to:
- sleep
- movement
- protein
- recovery
- stress management
- consistency
Peptides may support those goals.
But they cannot replace them.
The Importance Of Simplicity
The women who usually achieve the best long-term results are rarely the women doing:
- the most extreme stacks
- the most aggressive protocols
- endless experimentation
Instead, they tend to focus on:
- consistency
- realistic expectations
- sustainable routines
- gradual improvement
- recovery
- metabolic health
That’s the healthiest long-term mindset.
Safety & Professional Oversight
Because peptides can influence:
- metabolism
- hormones
- appetite
- recovery pathways
- growth signaling
…it’s important to approach stacking carefully.
Women should especially seek guidance if they have:
- hormone-sensitive conditions
- cancer histories
- metabolic disorders
- autoimmune conditions
- pregnancy or breastfeeding considerations
Quality and sourcing matter enormously.
So does realistic thinking.
Why Women Are Moving Toward Longevity Wellness
One of the healthiest things happening in modern wellness is that women are becoming less obsessed with:
- punishment
- perfection
- shrinking themselves
And more focused on:
- strength
- energy
- resilience
- confidence
- movement
- healthy aging
- quality of life
That shift changes everything.
Because wellness should ultimately help women:
feel more alive—not more exhausted.
Ava’s Perspective
If there’s one thing I’ve learned through exploring wellness and longevity, it’s this:
the body responds best to support—not war.
The women who thrive long-term are usually not the women punishing themselves constantly.
They’re the women who:
- recover properly
- nourish themselves well
- maintain muscle
- move consistently
- sleep deeply
- manage stress intelligently
- stay emotionally balanced
Peptides can sometimes support those goals.
But they work best when built on a strong foundation—not used as a substitute for one.
And honestly, I think that’s the healthiest possible way to approach modern wellness.
Key Takeaways
Wellness should focus on vitality, resilience, and quality of life—not punishment or perfection.
Peptide stacking means combining peptides with complementary wellness goals.
Common stack categories include metabolism, recovery, sleep, longevity, and regenerative wellness.
More compounds do not automatically create better results.
Recovery and muscle preservation remain foundational for healthy aging.
Sustainable wellness depends more on consistency than extreme optimization.
Quality sourcing and professional oversight matter enormously.
Early Signs of Magnesium Deficiency and Natural Ways to Restore Healthy Levels
Early Signs of Magnesium Deficiency and Natural Ways to Restore Healthy Levels
Magnesium is a major mineral your body needs every day. It helps support normal muscle contraction, nerve signaling, heart rhythm, bone health, blood sugar regulation, and the production of cellular energy.
A true magnesium deficiency is not always obvious at first. Mild low magnesium may cause vague symptoms, and blood magnesium tests do not always reflect total body magnesium stores. Still, recognizing possible magnesium deficiency signs can help you know when to review your diet, medications, health conditions, and supplement needs with a healthcare professional.
Common early signs of magnesium deficiency
Early magnesium deficiency symptoms may be subtle. Possible signs include:
- Muscle twitches, cramps, or spasms
- Fatigue or low energy
- Weakness
- Nausea or reduced appetite
- Headaches in some people
- Trouble sleeping or restless feelings
- Tingling or numbness
- Irritability or mood changes
- Heart palpitations or abnormal heartbeat sensations
These symptoms can have many causes, so they do not automatically mean you are magnesium deficient. However, they may be worth discussing with a clinician, especially if you have risk factors.
More serious signs that need medical attention
More severe magnesium deficiency can affect the nervous system, muscles, and heart. Seek medical care promptly if you experience:
- Persistent or severe muscle cramps or weakness
- Confusion, seizures, or significant neurological symptoms
- Fainting, chest pain, or shortness of breath
- Irregular heartbeat or strong palpitations
- Ongoing vomiting or diarrhea
- Symptoms after heavy alcohol use or while taking medications that affect minerals
Severe magnesium deficiency can occur with other electrolyte problems, including low potassium or low calcium, and may require medical treatment.
Why magnesium levels can become low
Magnesium deficiency may happen when intake is too low, absorption is poor, or losses are increased. Common contributors include:
- Diets low in nuts, seeds, legumes, whole grains, and leafy greens
- Long-term gastrointestinal conditions such as Crohn disease, celiac disease, or chronic diarrhea
- Heavy alcohol use
- Poorly controlled diabetes
- Older age
- Certain medications, including some diuretics, proton pump inhibitors, and some antibiotics or chemotherapy drugs
- Kidney-related mineral handling problems
If you take prescription medications, do not stop them on your own. Ask your healthcare provider whether they could affect magnesium status.
Natural ways to restore healthy magnesium levels
1. Eat more magnesium-rich foods
Food is usually the best first step for supporting magnesium intake. Good sources include:
- Pumpkin seeds, chia seeds, flaxseeds, and sesame seeds
- Almonds, cashews, and peanuts
- Spinach, Swiss chard, and other leafy greens
- Black beans, kidney beans, chickpeas, lentils, and soy foods
- Oats, brown rice, quinoa, and whole wheat products
- Avocado and bananas
- Plain yogurt and milk
- Dark chocolate with a high cocoa content
A simple magnesium-supportive meal could include a spinach and black bean bowl with brown rice, avocado, pumpkin seeds, and a yogurt-based dressing.
2. Improve overall mineral balance
Magnesium works closely with potassium, calcium, and vitamin D. A balanced diet with fruits, vegetables, beans, nuts, seeds, dairy or fortified alternatives, and whole grains helps support overall electrolyte and bone health.
3. Address digestive issues
Chronic diarrhea, malabsorption, inflammatory bowel disease, celiac disease, and some weight-loss surgeries can reduce magnesium absorption. If you have ongoing digestive symptoms, testing and medical guidance are important.
4. Review medications with your clinician
Some medications can increase magnesium loss or reduce magnesium levels over time. Long-term proton pump inhibitor use and certain diuretics are common examples. Your clinician may recommend monitoring, dietary changes, or supplementation depending on your situation.
5. Consider supplements only when appropriate
Magnesium supplements may help some people, but they are not risk-free. Too much supplemental magnesium can cause diarrhea, nausea, abdominal cramping, and, in high amounts, dangerous effects such as low blood pressure, irregular heartbeat, or confusion.
People with kidney disease should be especially cautious because the kidneys help remove excess magnesium. Always ask a healthcare professional before supplementing if you have kidney disease, heart disease, are pregnant, or take medications.
Common supplement forms include magnesium citrate, glycinate, oxide, and chloride. Tolerance and absorption can vary by form and dose.
How magnesium deficiency is diagnosed
Healthcare professionals may use a combination of symptom review, diet history, medication review, medical history, and blood tests. A standard serum magnesium test can detect low blood magnesium, but it may not fully represent magnesium stored in bone and tissues. In some cases, clinicians may also check calcium, potassium, kidney function, and other markers.
Key takeaways
Magnesium deficiency signs can include muscle cramps, twitching, fatigue, weakness, nausea, sleep difficulties, tingling, mood changes, and heart rhythm symptoms. The safest natural approach is to increase magnesium-rich whole foods, address digestive or medication-related causes, and seek medical guidance before using supplements, especially if symptoms are persistent or severe.
References
Chapter 15: Epitalon

Longevity, Sleep & The Search For Healthy Aging
Eventually, almost every wellness conversation leads to one unavoidable reality:
aging.
Not just appearance.
But deeper questions like:
- How do we preserve vitality?
- How do we maintain cognitive clarity?
- How do we stay resilient longer?
- How do we age without feeling physically diminished?
For many women, these questions become more meaningful during midlife.
Because aging stops feeling theoretical.
You begin noticing:
- changing recovery
- sleep disruption
- lower resilience
- hormonal shifts
- metabolic changes
- altered energy patterns
And often, women realize they are not necessarily afraid of getting older.
They are afraid of:
- losing vitality
- losing independence
- losing physical capability
- losing the feeling of being fully alive
This growing interest in:
- longevity
- biological aging
- cellular health
- resilience-focused wellness
is one reason discussions around:
Epitalon
have become increasingly popular in advanced longevity and biohacking circles.
What Is Epitalon?
Epitalon is a synthetic peptide originally studied in relation to:
- aging
- cellular health
- melatonin regulation
- sleep
- longevity-related biological processes
It became especially well known in longevity communities because of research involving:
- telomeres
- cellular aging pathways
- pineal gland function
- circadian rhythm regulation
That sounds highly technical, so let’s simplify it.
What Are Telomeres?
Telomeres are protective structures located at the ends of chromosomes.
They are often compared to:
the plastic tips on shoelaces.
Over time, telomeres naturally shorten as cells divide and age.
Researchers have explored whether telomere shortening may relate to:
- biological aging
- reduced cellular resilience
- age-related decline
This is one reason longevity science became fascinated with compounds potentially connected to:
- cellular repair
- aging pathways
- resilience mechanisms
Epitalon entered this conversation because of early research exploring its possible relationship to telomerase activity and cellular aging pathways.
Again:
much more research is still needed.
But the concept generated enormous interest in longevity-focused wellness communities.
Why Women Become Interested In Longevity Wellness
At some point, many women realize they care less about:
- looking younger
and more about: - feeling stronger
- thinking clearly
- maintaining independence
- preserving energy
- remaining physically capable
That’s an important emotional shift.
Because healthy aging is not really about vanity.
It’s about:
quality of life.
Women want to:
- travel comfortably
- stay active
- maintain cognitive sharpness
- feel resilient
- continue fully participating in life
That’s what makes longevity wellness so emotionally compelling.
The Sleep & Circadian Rhythm Connection
One reason Epitalon discussions became especially popular among women is its association with:
- sleep regulation
- melatonin-related pathways
- circadian rhythm support
And honestly:
sleep affects almost everything.
Poor sleep may contribute to:
- accelerated aging
- inflammation
- insulin resistance
- fatigue
- mood changes
- cognitive decline
- poor recovery
- hormonal disruption
Many women navigating midlife experience:
- lighter sleep
- waking during the night
- difficulty staying asleep
- reduced recovery from poor sleep
This is one reason sleep-focused longevity conversations have become so important.
Because sleep is one of the body’s most powerful recovery and repair systems.
Why Aging Feels Different For Women
Women often experience aging differently emotionally than men.
Many women simultaneously navigate:
- hormonal changes
- caregiving stress
- career pressure
- sleep disruption
- changing identity roles
- body composition shifts
And through all of this, they’re still expected to:
- perform
- care for others
- remain productive
- appear youthful
- stay energetic
That’s exhausting.
Which is one reason women are increasingly drawn toward wellness conversations focused on:
restoration instead of perfection.
Potential Benefits Women Commonly Discuss
Women exploring Epitalon discussions often mention goals such as:
- healthy aging support
- improved sleep quality
- recovery support
- circadian rhythm support
- longevity-focused wellness
- energy support
- resilience support
Some women also describe:
- feeling more rested
- improved recovery sensation
- improved sleep consistency
- greater interest in proactive aging strategies
Again, responses vary significantly and long-term research remains ongoing.
The Difference Between Lifespan & Healthspan
One of the most important ideas in longevity science is the distinction between:
lifespan
and
healthspan.
Lifespan simply means:
how long you live.
Healthspan means:
how well you live while aging.
Most women are not interested in:
- simply adding more years
if those years involve: - exhaustion
- frailty
- poor mobility
- cognitive decline
- chronic disease
Women increasingly want:
- vitality
- resilience
- mental clarity
- strength
- independence
for as long as possible.
That’s what healthy-aging conversations should really focus on.
The Wellness Industry’s Fear Problem
One thing I dislike about parts of the anti-aging industry is how heavily it relies on:
- fear
- insecurity
- panic around aging
But aging itself is not failure.
Aging is:
- biological
- natural
- inevitable
The healthier goal is not:
trying to stop aging.
The healthier goal is:
supporting the body intelligently while aging.
That mindset creates far healthier emotional relationships with wellness.
Common Wellness Pairings
In longevity-focused wellness circles, Epitalon is often discussed alongside:
- sleep optimization
- stress reduction
- metabolic health strategies
- recovery-focused wellness
- mitochondrial support
- movement routines
- anti-inflammatory nutrition
- nervous system regulation
Because ultimately:
longevity is rarely about one single intervention.
It’s usually the cumulative effect of:
- movement
- recovery
- sleep
- nutrition
- stress management
- metabolic health
- consistency
Side Effects & Considerations
Because long-term human data remains limited, side effects and risks continue being evaluated.
Potentially discussed side effects may include:
- fatigue
- headaches
- dizziness
- temporary sleep changes
- injection site irritation
Individual responses vary considerably.
Again, cautious optimism is healthier than exaggerated hype.
Contraindications & Unknowns
Women with:
- cancer histories
- complex medical conditions
- autoimmune disease
- pregnancy or breastfeeding considerations
should discuss any advanced longevity therapies carefully with qualified healthcare professionals.
Long-term human evidence remains limited.
That’s important to acknowledge honestly.
Why Women Are Rethinking Aging
One thing I find incredibly encouraging is that many women are redefining what aging means.
Instead of chasing impossible standards, more women are focusing on:
- energy
- movement
- resilience
- vitality
- emotional wellbeing
- longevity
- metabolic health
That’s a far healthier direction than:
fear-based anti-aging culture.
Because healthy aging is not about pretending you’re 25 forever.
It’s about:
remaining strong, capable, and fully alive throughout life.
The Truth About Longevity
The women who tend to age most powerfully are rarely the ones obsessing over perfection.
They are usually the women who:
- move consistently
- manage stress wisely
- maintain muscle
- prioritize sleep
- nourish themselves adequately
- cultivate purpose
- preserve curiosity
- stay socially connected
Longevity is deeply connected to:
how we live emotionally as well as physically.
That matters more than most people realize.
Ava’s Perspective
The older I get, the less interested I become in:
- looking younger
and the more interested I become in: - feeling vibrant
- staying capable
- preserving energy
- protecting my mind
- maintaining freedom and independence
To me, that’s what longevity should really mean.
Not fear of aging.
But respect for the body and life itself.
Aging gracefully is not weakness.
It’s wisdom.
And I think women become extraordinarily powerful when they stop viewing aging as something shameful and start viewing it as something to navigate intelligently and confidently instead.
Key Takeaways
Longevity wellness works best when rooted in sustainable lifestyle foundations.
Epitalon is commonly discussed in longevity and healthy-aging conversations.
Interest centers around sleep, circadian rhythm, and cellular aging pathways.
Women increasingly prioritize healthspan—not simply lifespan.
Sleep quality strongly affects aging, recovery, metabolism, and resilience.
Healthy aging should focus on vitality and independence rather than fear.
Long-term human research on Epitalon remains limited.
Chapter 14: GHK-Cu

Skin, Hair, Collagen & The Beauty-Longevity Connection
At some point in nearly every woman’s wellness journey, the conversation around aging becomes personal.
Not because women fear aging itself.
But because many women begin noticing subtle changes that affect how they feel about themselves:
- thinner skin
- slower healing
- reduced elasticity
- fine lines
- hair thinning
- dullness
- slower recovery after procedures
- changes in overall skin quality
And while social media often pushes extreme anti-aging messaging, most women are not trying to look 25 forever.
They simply want to:
- look healthy
- feel vibrant
- age gracefully
- maintain confidence
- feel like themselves
This is one reason interest exploded around:
GHK-Cu.
Unlike many peptides discussed for metabolism or recovery, GHK-Cu became especially popular in:
- skincare
- regenerative aesthetics
- longevity wellness
- hair restoration conversations
Because it sits at the intersection of:
beauty and biological repair.
What Is GHK-Cu?
GHK-Cu is a naturally occurring copper-binding peptide found in the human body.
It has been studied for its relationship to:
- collagen production
- tissue repair
- skin regeneration
- wound healing
- hair-related wellness
- inflammatory signaling
Levels of naturally occurring GHK-Cu decline with age.
This decline is one reason it became increasingly interesting within:
- longevity science
- regenerative medicine
- advanced skincare conversations
Why Women Become Interested In It
For many women, aging is not simply about appearance.
It’s about:
- confidence
- vitality
- self-recognition
- feeling healthy
- looking rested
- feeling feminine and strong simultaneously
Women often describe wanting to:
- age naturally
- avoid looking “overdone”
- maintain healthy skin quality
- support collagen
- preserve hair thickness
- improve overall skin vitality
This is one reason peptides associated with:
- regeneration
- collagen support
- skin quality
became so popular.
Especially among women seeking:
graceful aging instead of artificial perfection.
The Skin & Longevity Connection
One thing I find fascinating is that skin often reflects what’s happening internally.
Skin quality can be influenced by:
- inflammation
- stress
- sleep
- hormones
- nutrition
- blood sugar stability
- recovery
- collagen production
- overall metabolic health
Which means skin health is not only cosmetic.
It’s connected to broader biological wellness.
This is why regenerative skincare conversations increasingly overlap with:
longevity and wellness discussions.
How GHK-Cu Is Thought To Work
Research surrounding GHK-Cu suggests it may influence pathways associated with:
- collagen synthesis
- tissue repair
- skin remodeling
- inflammatory regulation
- wound healing
- antioxidant activity
Some research has explored its relationship to:
- skin firmness
- elasticity
- recovery after cosmetic procedures
- hair-related wellness support
Again, while research is promising in several areas, long-term large-scale human evidence continues evolving.
Balanced expectations matter.
Why Collagen Matters So Much
Collagen is one of the structural proteins responsible for:
- skin firmness
- elasticity
- connective tissue integrity
- healthy aging appearance
As women age, collagen production naturally declines.
This contributes to:
- thinner skin
- fine lines
- reduced elasticity
- slower healing
- visible aging changes
Hormonal transitions may accelerate some of these changes even further.
Which is one reason many women begin prioritizing:
skin quality rather than simply covering signs of aging.
Hair Loss & Midlife Confidence
One topic women often discuss quietly—but deeply emotionally—is hair thinning.
Hormonal changes, stress, inflammation, and aging may all contribute to:
- thinning hair
- reduced fullness
- slower growth
- texture changes
And because hair is closely connected to identity and femininity for many women, these changes can feel surprisingly emotional.
This is one reason regenerative wellness conversations involving:
- scalp health
- hair vitality
- collagen support
- recovery signaling
have become increasingly popular.
Potential Benefits Women Commonly Discuss
Women exploring GHK-Cu often discuss goals such as:
- improved skin quality
- collagen support
- healthier-looking skin
- improved elasticity
- recovery support after cosmetic procedures
- hair vitality support
- healthy-aging skincare
- reduced visible signs of aging
Some women also describe:
- improved confidence
- healthier overall appearance
- skin looking more “rested”
- improved glow and texture
Again, responses vary significantly between individuals.
Beauty & Wellness Shouldn’t Feel Opposed
One thing I believe strongly is this:
wanting to look good is not shallow.
Women are often made to feel guilty for caring about appearance.
But there’s nothing wrong with wanting to:
- feel attractive
- feel confident
- feel vibrant
- maintain healthy skin
- preserve femininity
The healthiest approach is not obsession.
It’s balance.
And I think modern wellness becomes much healthier when we stop pretending women must choose between:
- self-care
and - self-acceptance.
Both can coexist beautifully.
The Problem With Extreme Anti-Aging Culture
Modern beauty culture often promotes:
- fear of aging
- unrealistic perfection
- constant comparison
- cosmetic obsession
But true longevity wellness should not create shame around aging.
Healthy aging should mean:
- supporting the body
- maintaining vitality
- improving resilience
- preserving confidence
- caring for yourself intentionally
That’s a much healthier emotional framework than:
desperately trying to erase time.
Common Wellness Pairings
In regenerative wellness conversations, GHK-Cu is often discussed alongside:
- collagen-supportive nutrition
- sleep optimization
- hydration
- antioxidant-focused wellness
- skin-recovery routines
- strength training
- blood sugar management
- anti-inflammatory lifestyles
Because ultimately:
skin health reflects overall health more than most people realize.
Side Effects & Considerations
Depending on the form used, side effects discussed may include:
- skin irritation
- redness
- sensitivity
- temporary reactions at application sites
- headaches
- irritation from topical products
Responses vary depending on:
- formulation quality
- delivery method
- individual sensitivity
Contraindications & Unknowns
Women with:
- copper metabolism disorders
- significant dermatologic conditions
- pregnancy or breastfeeding considerations
- complex medical histories
should discuss advanced regenerative therapies carefully with qualified professionals.
Again:
quality matters enormously.
Especially in regenerative wellness and skincare products.
The Bigger Emotional Shift
What I find most encouraging about modern longevity wellness is that many women are shifting away from:
- punishing beauty standards
- crash dieting
- obsessive anti-aging culture
And toward:
- nourishment
- vitality
- skin health
- movement
- confidence
- graceful aging
That’s an incredibly healthy evolution.
Because ultimately, the goal should not be:
looking artificially young.
The goal should be:
looking healthy, vibrant, and alive.
Aging Gracefully Is Powerful
One thing I’ve realized over time is that confidence does not come from perfection.
It comes from:
- vitality
- energy
- self-respect
- resilience
- authenticity
- feeling good in your own skin
Women do not become less valuable as they age.
In many ways, they become:
- wiser
- stronger
- more grounded
- more self-aware
Healthy aging should support that evolution—not create fear around it.
Ava’s Perspective
I think one of the most beautiful things a woman can do is care for herself intentionally without becoming consumed by perfection.
To me, healthy aging means:
- nourishing your body
- protecting your energy
- preserving your confidence
- supporting your skin and health
- maintaining vitality
- continuing to feel feminine and strong
Not chasing impossible standards.
Just becoming:
the healthiest, strongest version of yourself at every stage of life.
And honestly, I think that mindset is far more attractive than perfection ever could be.
Key Takeaways
- GHK-Cu is commonly discussed for collagen, skin, and regenerative wellness support.
- Skin health reflects broader metabolic and inflammatory health.
- Many women seek graceful aging—not artificial perfection.
- Collagen production naturally declines with age.
- Confidence and self-care can coexist with healthy self-acceptance.
- Regenerative wellness should support vitality rather than fear-based anti-aging.
Healthy aging is about looking and feeling vibrant, resilient, and alive.
Chapter 13: Thymosin Beta-4 (TB-500)

Recovery, Mobility & The “Feel Younger Again” Peptide
One of the hardest parts of aging for many women is not appearance.
It’s limitation.
The feeling that your body no longer responds the way it once did.
The realization that:
- recovery takes longer
- injuries linger
- inflammation sticks around
- mobility decreases
- workouts feel harder
- soreness becomes constant
And over time, this can quietly chip away at confidence.
Many women stop doing things they once loved because movement no longer feels effortless:
- hiking
- strength training
- tennis
- yoga
- long walks
- dancing
- simply feeling physically capable
This is one reason recovery-focused peptides have become such a major area of interest in longevity wellness.
And among them, one peptide appears constantly in conversations around:
- recovery
- healing
- mobility
- inflammation support
- physical resilience
TB-500.
What Is TB-500?
TB-500 is a synthetic version of a naturally occurring peptide called:
Thymosin Beta-4.
This peptide is involved in processes related to:
- tissue repair
- cellular migration
- recovery
- inflammation regulation
- wound healing
In wellness and athletic communities, TB-500 is often discussed for:
- mobility support
- soft tissue recovery
- inflammation reduction
- workout recovery
- injury-related recovery conversations
Especially among individuals trying to remain:
- active
- strong
- physically resilient as they age.
Why Women Become Interested In Recovery Peptides
For many women over 35, the issue is not lack of motivation.
It’s that the body becomes less forgiving.
Women often notice:
- longer recovery times
- chronic stiffness
- recurring injuries
- joint discomfort
- exercise fatigue
- reduced mobility
And eventually many women stop exercising consistently not because they’re lazy, but because:
movement stopped feeling good.
That distinction matters.
Because physical discomfort affects:
- consistency
- motivation
- energy
- confidence
- emotional wellbeing
This is one reason recovery and mobility conversations have become increasingly important in women’s wellness.
Why Mobility Matters More Than Women Realize
One thing I believe strongly is this:
mobility is freedom.
When the body moves comfortably:
- confidence improves
- movement becomes enjoyable
- exercise becomes sustainable
- energy improves
- life expands
But when pain, stiffness, or inflammation increase, life often begins shrinking:
- less movement
- less spontaneity
- less confidence
- less vitality
That’s why mobility-focused wellness matters so much.
Not because women are chasing perfection.
But because they want to:
- remain capable
- remain independent
- remain active
- continue enjoying life physically
How TB-500 Is Thought To Work
Research surrounding TB-500 is still developing, but it is believed to influence processes associated with:
- tissue repair
- inflammation regulation
- recovery signaling
- cellular movement during healing processes
Animal and preclinical studies have generated interest around:
- tendon healing
- muscle recovery
- wound repair
- inflammation modulation
Again, it’s important to understand:
long-term human research remains limited.
Much of the excitement surrounding TB-500 comes from:
- early research
- athletic communities
- anecdotal experiences
- longevity-focused wellness discussions
Balanced expectations remain important.
Why Inflammation Changes Everything
Chronic inflammation affects far more than appearance or soreness.
It may influence:
- energy
- recovery
- sleep
- metabolism
- mobility
- cognitive clarity
- exercise consistency
And unfortunately, modern life often creates an inflammatory environment through:
- stress
- poor sleep
- processed foods
- sedentary behavior
- blood sugar instability
- overtraining
- hormonal changes
This is one reason recovery and inflammation support have become central topics in healthy-aging conversations.
Women increasingly realize:
longevity is not just about living longer.
It’s about feeling functional while living longer.
Potential Benefits Women Commonly Discuss
Women exploring TB-500 often discuss goals such as:
- improved recovery
- reduced soreness
- mobility support
- inflammation reduction
- soft tissue support
- exercise resilience
- physical longevity
- improved movement comfort
Some women also report:
- greater confidence exercising again
- feeling less physically fragile
- improved consistency with movement routines
- improved recovery after activity
Again, experiences vary significantly between individuals.
The Emotional Side Of Physical Decline
One thing that often goes unspoken is how emotionally difficult it can feel when your body stops cooperating.
Many women quietly grieve:
- loss of athleticism
- reduced stamina
- chronic discomfort
- fear of injury
- feeling older physically
Not because they expect perfection.
But because they miss:
- feeling strong
- feeling capable
- feeling energized
- feeling physically free
That emotional experience deserves compassion—not shame.
Recovery Is Becoming A Wellness Priority
One of the healthiest shifts happening in modern wellness is that women are finally recognizing:
recovery is productive.
For years, wellness culture glorified:
- exhaustion
- overtraining
- restriction
- burnout
- pushing harder constantly
But eventually, many women realize the body thrives more from:
- restoration
- sleep
- mobility
- nourishment
- recovery
- nervous system regulation
That’s not weakness.
That’s intelligent aging.
Common Wellness Pairings
In longevity and recovery-focused conversations, TB-500 is often discussed alongside:
- mobility training
- physical therapy
- strength training
- walking
- anti-inflammatory nutrition
- recovery protocols
- flexibility work
- sleep optimization
Women interested in these discussions are often focused on:
maintaining physical capability long-term.
Side Effects & Considerations
Potential side effects discussed anecdotally may include:
- fatigue
- headaches
- nausea
- dizziness
- injection site irritation
- temporary discomfort
Because long-term human research remains limited, caution and quality sourcing matter enormously.
Contraindications & Unknowns
Women with:
- cancer histories
- autoimmune conditions
- complex medical conditions
- pregnancy or breastfeeding considerations
should discuss any recovery-related peptide exploration carefully with qualified healthcare professionals.
As with many emerging peptides:
long-term evidence continues evolving.
The Bigger Longevity Conversation
What I find most interesting about recovery peptides is that they reflect a broader shift in women’s wellness priorities.
Women are becoming less obsessed with:
- punishing workouts
- shrinking themselves
- chasing unrealistic perfection
And more interested in:
- strength
- movement
- mobility
- resilience
- vitality
- quality of life
That’s a profoundly healthier direction.
Because ultimately, healthy aging is not about looking untouched by time.
It’s about:
continuing to fully participate in life.
The Connection Between Movement & Confidence
One thing I’ve noticed repeatedly is that movement affects confidence deeply.
When women feel physically strong and capable:
- posture changes
- mood improves
- energy improves
- resilience improves
- life expands
But when movement becomes painful or difficult, confidence often quietly declines too.
That’s why recovery matters emotionally—not just physically.
Ava’s Perspective
The older I get, the more I value:
feeling physically capable.
Not perfect.
Not flawless.
Just capable.
Able to:
- move comfortably
- exercise consistently
- recover well
- travel easily
- enjoy life physically
To me, that’s what longevity should actually mean.
Not obsessing over youth.
But preserving:
- movement
- resilience
- vitality
- independence
- confidence in your body
And honestly, I think that’s a far healthier goal than most modern wellness culture promotes.
Key Takeaways
Healthy aging should prioritize strength, movement, resilience, and physical freedom.
TB-500 is commonly discussed for recovery, mobility, and inflammation support.
Recovery and physical resilience become increasingly important after 35.
Mobility strongly affects confidence, energy, and quality of life.
Chronic inflammation can impact recovery, metabolism, and vitality.
Modern wellness is shifting toward restoration rather than burnout.
Long-term human research on TB-500 remains limited.
.